Think of a city that never shuts down. It’s always active, always moving. To stay alive, it needs nonstop deliveries of food, water, and oxygen. At the same time, waste has to be cleared fast and efficiently. Inside our body, that city is made up of organs and tissues. The system that keeps everything running is the cardiovascular system.
This system is a powerful, nonstop network of the heart, blood, and blood vessels. It works day and night without breaks. Every second, it delivers oxygen and nutrients to our cells, from our brain down to our toes. It also carries away waste before it can cause harm. Without this system, the body would shut down within minutes.
In this guide, we’ll take a clear and simple journey through this inner highway. First, we’ll look at the structure of the heart and how it works. Then, we’ll explore the different types of blood vessels and their roles. After that, we’ll break down the cardiac cycle and its steady rhythm. Finally, we’ll see how our body controls blood pressure to keep us active, balanced, and full of energy.
What is the cardiovascular system?
The cardiovascular system, often called the circulatory system, works like the body’s main delivery network. Its core job is simple but powerful: move fluids through the body in a continuous, closed loop under pressure. At first, it may sound like it’s all about the heart. However, the system only works because three key parts operate together. Think of it as a well-coordinated team.
First, there is the pump. The heart generates the force that keeps everything moving. Next comes the fluid. Blood carries oxygen, nutrients, hormones, and waste from one place to another. Finally, there are the pipes. Blood vessels—arteries, veins, and capillaries—form the pathways that guide blood throughout the body. Together, these three components keep life flowing, second by second.
Why It Is Essential for Life
The cardiovascular system serves as the body’s ultimate multitasker. Its primary role is homeostasis—the maintenance of a stable internal environment. It achieves this through:
- Oxygen Delivery: Picking up oxygen from the lungs and delivering it to tissues.
- Nutrient Transport: Carrying glucose, amino acids, and fats from the digestive tract to the cells.
- Waste Removal: Transporting carbon dioxide to the lungs and metabolic waste to the kidneys.
- Hormone Signaling: Acting as a “postal service” for hormones like adrenaline and insulin.
- Temperature Regulation: Shifting blood flow to the skin to cool down or keeping it in the core to stay warm.
Blood: The Life-Sustaining Fluid of the Cardiovascular System
What Makes Blood So Special?
Blood is far more than just a red liquid flowing through our veins. It’s a living tissue composed of cells suspended in a liquid called plasma. If you were to separate blood in a test tube, you’d see it naturally divides into layers, revealing its hidden complexity.
Composition: Cells + Plasma
Plasma makes up about 55% of our blood volume. This yellowish fluid is mostly water (around 90%), but it’s packed with dissolved proteins, glucose, hormones, electrolytes, and clotting factors. Think of plasma as the delivery truck that carries everything our cells need. The remaining 45% consists of cellular components:
- Red blood cells (erythrocytes) are the most abundant, numbering around 5 million per microliter. These disk-shaped cells are loaded with hemoglobin, a protein that binds oxygen in our lungs and releases it throughout our body. Their unique biconcave shape maximizes surface area for gas exchange.
- White blood cells (leukocytes) are our immune system’s soldiers. Though far less numerous than red cells, they patrol our bloodstream hunting for bacteria, viruses, and other invaders.
- Platelets (thrombocytes) are tiny cell fragments that rush to injury sites to form clots and stop bleeding. Without them, even a small cut could be life-threatening.
Functions: Transport, Immunity, and Regulation
Blood performs three critical jobs simultaneously:
- Transportation is the primary function. Oxygenated blood carries fresh oxygen from your lungs to every cell. On the return trip, deoxygenated blood collects carbon dioxide waste for disposal. Blood also delivers nutrients from our digestive system, hormones from glands, and heat from active muscles to cooler body regions.
- Protection comes from your white blood cells and antibodies floating in plasma. They identify threats, neutralize toxins, and remember past infections to respond faster next time.
- Regulation maintains your body’s delicate balance. Blood helps control our pH levels, body temperature, and fluid balance between tissues. When you’re overheating during exercise, blood vessels near your skin dilate to release excess heat.
Heart Anatomy—The Central Pump
Our heart sits in our chest cavity, slightly left of center, nestled between our lungs. About the size of our fist, it beats approximately 100,000 times daily, pumping blood with remarkable efficiency.
Three protective layers shield this vital organ:
The pericardium is the tough outer sac that anchors our heart and prevents overfilling. It’s like a protective sleeping bag that holds our heart in place while allowing movement.
The myocardium is the thick muscular middle layer that does the actual pumping. These specialized cardiac muscle cells contract in perfect coordination, generating the force needed to push blood throughout our entire body.
The endocardium is the smooth inner lining that prevents blood from sticking to the heart walls. This slick surface ensures blood flows smoothly without clotting.
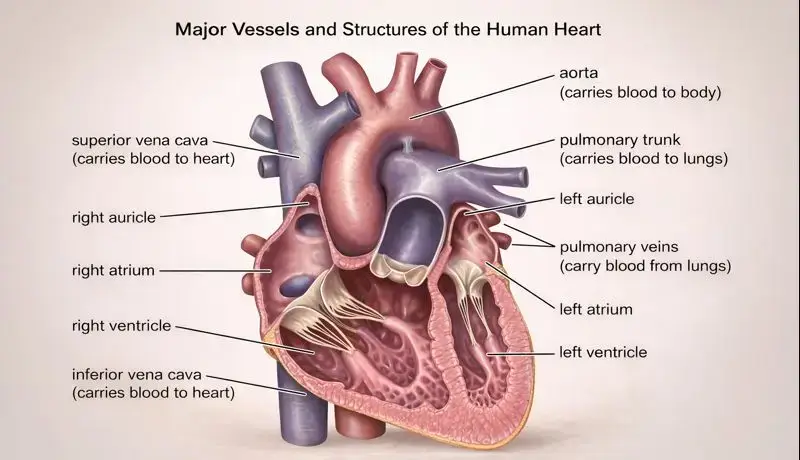
Chambers and Valves: The Four-Room Design
Our heart functions as two pumps working side by side, divided into four chambers:
The right atrium receives deoxygenated blood returning from our body through two large veins called the superior and inferior vena cavae. This thin-walled chamber acts as a receiving room.
The right ventricle pumps this oxygen-poor blood to our lungs through the pulmonary arteries. It doesn’t need to generate as much pressure since the lungs are nearby.
The left atrium receives freshly oxygenated blood from our lungs via four pulmonary veins. Again, it’s a temporary holding chamber.
The left ventricle is the powerhouse. Its thick, muscular walls generate enough force to send blood on a journey through our entire body. This chamber works the hardest and is prone to problems when blood pressure stays elevated.
Four valves act as one-way doors, ensuring blood flows in the right direction:
- Tricuspid valve (between right atrium and ventricle)
- Pulmonary valve (between right ventricle and pulmonary artery)
- Mitral valve (between left atrium and ventricle)
- Aortic valve (between left ventricle and aorta)
When these valves malfunction, you might hear a heart murmur—the sound of blood flowing backward or through a narrowed opening.
Major Vessels: The Highway Connections
The aorta is our body’s main artery, emerging from the left ventricle. This massive vessel branches into smaller arteries that reach every corner of our body, from our brain to our toes.
The vena cavae are the two largest veins returning blood to the heart. The superior vena cava drains our upper body, while the inferior vena cava handles everything below our heart.
The pulmonary arteries carry deoxygenated blood from our right ventricle to both lungs. Interestingly, these are the only arteries in our body that carry oxygen-poor blood.
The pulmonary veins return oxygenated blood from our lungs to the left atrium, completing the pulmonary circuit.
Blood Vessels and Circuits
Arteries vs. Veins vs. Capillaries
Our circulatory system anatomy includes three types of blood vessels, each designed for specific tasks:
Arteries are thick-walled, muscular vessels that carry blood away from our heart. They must withstand high pressure, so their walls contain elastic fibers and smooth muscle. You can feel an artery’s pulse because it expands slightly with each heartbeat. The largest arteries branch into smaller arterioles that control blood flow to different organs.
Veins return blood to our heart under much lower pressure. Their walls are thinner and less elastic than arteries. Many veins, especially in our legs, contain one-way valves that prevent backward flow when we’re standing. When these valves weaken, we develop varicose veins.
Capillaries are microscopic vessels where the real action happens. Their walls are just one cell thick, allowing oxygen, nutrients, and waste products to pass between blood and tissues. Every cell in our body sits within a hair’s breadth of a capillary.
Pulmonary vs. Systemic Circuits
Our cardiovascular system operates as two connected loops:
Pulmonary circulation is the shorter loop between our heart and lungs. Deoxygenated blood flows from the right ventricle through pulmonary arteries to our lungs. There, it releases carbon dioxide and picks up fresh oxygen. The newly oxygenated blood returns through pulmonary veins to the left atrium. This entire trip takes just a few seconds.
Systemic circulation is the longer loop serving our entire body. Oxygenated blood leaves the left ventricle through the aorta, traveling through progressively smaller arteries and arterioles until reaching capillary beds in our tissues. After exchanging oxygen for carbon dioxide, the now-deoxygenated blood begins its return journey through venules and veins, eventually reaching the right atrium via the vena cavae.
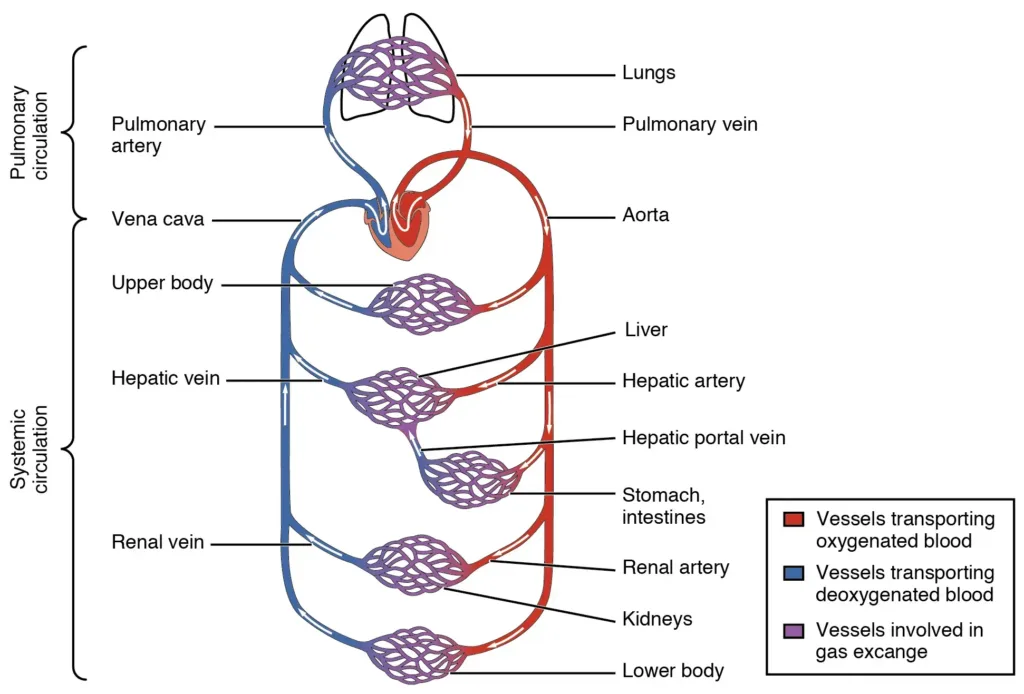
Vessel Hierarchy and Oxygenation
Think of our blood vessels as a branching tree. The aorta is the trunk, major arteries are large branches, arterioles are smaller twigs, and capillaries are the leaves where gas exchange occurs.
The fascinating part? Blood color changes with oxygenation. Oxygenated blood in arteries appears bright red because oxygen-bound hemoglobin reflects light differently. Deoxygenated blood in veins looks darker, almost purplish. Our veins appear blue through our skin due to how light penetrates and reflects through tissue, not because blood is actually blue.
Cardiac Cycle in Depth
Understanding the cardiac cycle explained means following one complete heartbeat from start to finish. This rhythmic sequence repeats about 70 times per minute at rest.
Phases: Diastole and Systole
Diastole is the relaxation phase when chambers fill with blood. It actually takes up about two-thirds of each cardiac cycle. During ventricular diastole, the ventricles relax and expand, creating negative pressure that sucks blood in from the atria. The atrioventricular valves (tricuspid and mitral) open passively, allowing blood to flow from atria into ventricles.
Systole is the contraction phase when chambers pump blood forward. Atrial systole gives the ventricles a final “topping off” before ventricular contraction begins. Then ventricular systole generates the force needed to eject blood—the right ventricle sends blood to the lungs while the left ventricle propels it throughout our body.
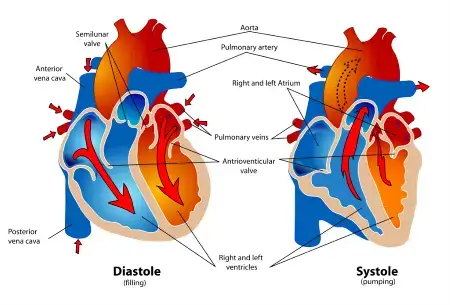
Pressure Changes Drive Flow
Blood flows from high pressure to low pressure, and the cardiac cycle creates these pressure gradients:
During diastole, ventricular pressure drops below atrial pressure, opening the AV valves. Blood flows passively into relaxed ventricles.
As systole begins, ventricular pressure skyrockets as the muscular walls contract. When ventricular pressure exceeds atrial pressure, the AV valves slam shut (creating the “lub” sound). As pressure continues rising, it eventually surpasses the pressure in the arteries, forcing open the semilunar valves (pulmonary and aortic).
Blood rushes out into the arteries until ventricular pressure falls during relaxation. When arterial pressure becomes higher than ventricular pressure, the semilunar valves close (creating the “dub” sound). The cycle begins again.
Volume Changes Mirror Pressure
The volume of blood in each ventricle changes throughout the cycle:
End-diastolic volume (EDV) is the maximum amount of blood in the ventricle after filling—typically around 120 milliliters.
End-systolic volume (ESV) is what remains after contraction—usually about 50 milliliters.
The difference between these two (EDV minus ESV) is our stroke volume—the amount pumped per beat. A healthy heart ejects roughly 70 milliliters per beat at rest. Multiply stroke volume by heart rate, and we get cardiac output: the total volume pumped per minute, typically 5 liters.
For readers wanting to explore heart physiology more deeply, “The Heart: An Introduction to Cardiovascular Physiology” offers detailed explanations with helpful illustrations that complement this overview.
Electrical Conduction System
Our heart has its own electrical system—a network of specialized cells that generates and coordinates every heartbeat without conscious input from our brain.
SA Node: The Natural Pacemaker
The sinoatrial (SA) node sits in the wall of our right atrium. These specialized cells spontaneously generate electrical impulses 60-100 times per minute, setting our resting heart rate. Think of the SA node as the conductor of an orchestra, establishing the tempo for all other cardiac cells to follow.
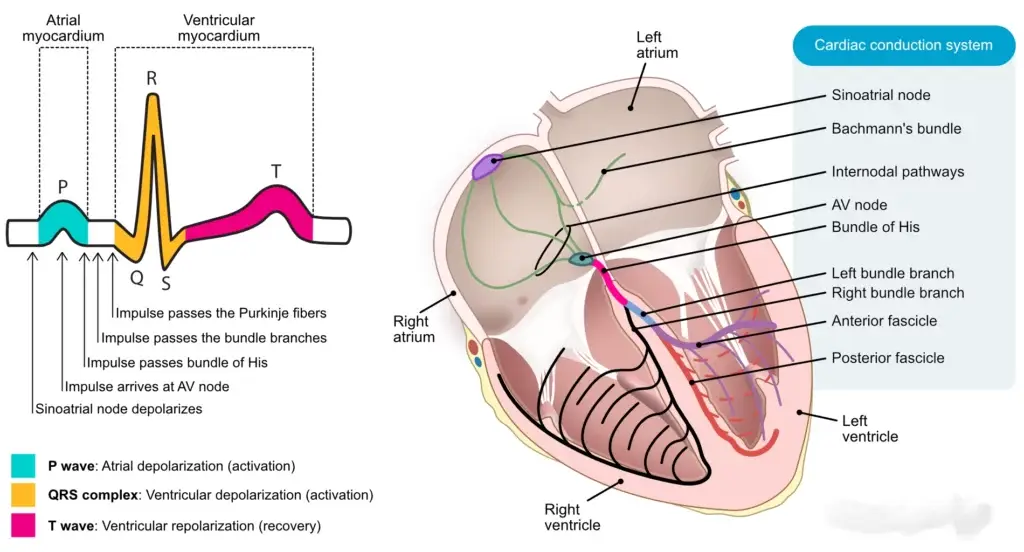
When the SA node fires, an electrical wave spreads across both atria like ripples on water, causing them to contract simultaneously. This electrical activity creates the P wave on an electrocardiogram (ECG).
AV Node: The Strategic Delay
The electrical signal reaches the atrioventricular (AV) node, located between the atria and ventricles. Here’s where something clever happens: the AV node delays the signal for about 0.1 seconds.
Why the pause? This delay ensures the atria finish contracting and emptying their blood into the ventricles before ventricular contraction begins. Without this timing, both chambers would contract simultaneously, reducing pumping efficiency dramatically.
This delay shows up as the flat PR segment on an ECG.
His-Purkinje Network: Rapid Distribution
After the delay, the signal travels through the bundle of His, which divides into right and left bundle branches running down both sides of the interventricular septum (the wall between ventricles).
These branches split into the Purkinje fibers—a network of specialized conducting cells that spread rapidly across the ventricular walls. This system allows both ventricles to contract almost simultaneously from the bottom up, efficiently squeezing blood upward into the arteries.
This ventricular depolarization creates the prominent QRS complex on an ECG.
ECG Basics: Reading Your Heart’s Electricity
An electrocardiogram traces your heart’s electrical activity through electrodes on your skin. Understanding the basic waves helps you appreciate what’s happening:
- P wave: Atrial depolarization (contraction)
- QRS complex: Ventricular depolarization (contraction)
- T wave: Ventricular repolarization (relaxation and recharging)
Doctors analyze these patterns to detect arrhythmias, heart attacks, and other electrical problems. An abnormally fast heartbeat (tachycardia), slow heartbeat (bradycardia), or irregular rhythm (like atrial fibrillation) shows up as distinctive ECG patterns.
Hemodynamics and Blood Pressure
Hemodynamics is the study of blood flow—how blood moves through our vessels and what factors influence that movement.
What Influences Flow?
Several interconnected factors determine how easily blood flows:
Blood vessel diameter is the most powerful factor. When a vessel’s radius doubles, flow increases by 16 times. This is why our arterioles (small arteries) are called “resistance vessels”—tiny changes in their diameter dramatically affect blood flow to organs.
Blood viscosity (thickness) affects flow resistance. Thicker blood flows more slowly. Conditions that increase red blood cell count make blood more viscous and harder to pump.
Vessel length matters too, though it doesn’t change much in adults. Taller people have slightly higher blood pressure because their hearts must pump blood farther against gravity.
Blood pressure regulation ensures adequate flow despite these variables. Our body constantly adjusts vessel diameter and heart output to maintain perfusion to vital organs.
Pressure Gradients: The Driving Force
Blood flows from areas of high pressure to low pressure. The pressure is highest in the aorta (around 120 mmHg during systole) and gradually decreases as blood travels through smaller vessels. By the time blood reaches the vena cavae, pressure has dropped to nearly 0 mmHg.
This pressure gradient is essential. Without it, blood would pool in our arteries instead of circulating. When you stand up quickly, gravity temporarily reduces pressure in our brain’s blood vessels, causing momentary dizziness until your body compensates.
Regulation: Baroreceptors and Hormones
Our body monitors and adjusts blood pressure constantly through multiple mechanisms:
Baroreceptors are stretch sensors in our aorta and carotid arteries. When they detect high pressure, they signal our brain to slow our heart rate and dilate blood vessels. Low-pressure triggers the opposite response.
Hormonal control provides longer-term regulation. When blood pressure drops, our kidneys release renin, triggering a cascade that produces angiotensin II—a powerful vasoconstrictor. This system also increases aldosterone release, which makes our kidneys retain more sodium and water, increasing blood volume and pressure.
Antidiuretic hormone (ADH) also helps by making our kidneys conserve water when we’re dehydrated, maintaining blood volume and pressure.
During exercise, these systems work together. Our heart rate jumps, vessels in working muscles dilate, vessels in our digestive system constrict, and blood pressure rises to meet increased oxygen demand.
Microcirculation and Gas Exchange
While arteries and veins transport blood, the real magic happens in our capillaries—the smallest and most numerous blood vessels in our body.
Capillary Exchange Mechanisms
Our approximately 10 billion capillaries create about 600 square meters of exchange surface. Their walls are just one cell thick, allowing substances to pass through via three main mechanisms:
Diffusion moves most substances. Oxygen and carbon dioxide simply flow down their concentration gradients—oxygen moving from blood into tissues, CO₂ moving from tissues into blood. This passive process requires no energy.
Filtration pushes fluid and small solutes out of capillaries at the arterial end, where pressure is higher. This fluid bathes tissues with nutrients and oxygen.
Reabsorption pulls fluid back into capillaries at the venous end, where pressure is lower. Proteins in blood plasma create osmotic pressure that draws about 85% of the filtered fluid back. The remaining 15% enters lymphatic vessels, eventually returning to our bloodstream.
Oxygen and CO₂ Diffusion
In our lungs, oxygen diffuses from air in alveoli (tiny air sacs) into pulmonary capillaries. Hemoglobin in red blood cells eagerly binds oxygen, turning blood bright red.
This oxygenated blood travels to systemic capillaries, where the reverse occurs. Cells have consumed their oxygen and produced CO₂, so oxygen concentration is low and CO₂ is high. Oxygen releases from hemoglobin and diffuses into cells, while CO₂ diffuses into blood for transport back to lungs.
Hemoglobin carries about 98% of oxygen. The remaining 2% dissolves directly in plasma. Carbon dioxide transport is more complex—about 70% converts to bicarbonate ions, 23% binds to hemoglobin, and 7% dissolves in plasma.
Nutrient and Waste Exchange
Besides gases, capillaries exchange countless other substances:
Nutrients like glucose, amino acids, fatty acids, and vitamins diffuse from blood into cells. After a meal, glucose levels spike, and cells throughout our body absorb what they need.
Wastes like urea, creatinine, and lactic acid move from cells into blood for elimination. Our kidneys filter these wastes from blood and excrete them in urine.
Hormones released by glands enter capillaries and travel to target organs. This is how our pancreas sends insulin to muscles and the liver after we eat.
This microscopic exchange sustains every cell in our body. Without functioning capillaries, cells would starve and suffocate within their own waste products.
Communication and Control
Our cardiovascular system doesn’t operate in isolation. It receives constant input from our nervous and endocrine systems, adjusting output to match our body’s changing needs.
Nervous System Role
The autonomic nervous system controls our heart and blood vessels without conscious thought. It has two divisions with opposing effects:
Sympathetic nerves prepare you for action. When you’re stressed, exercising, or facing danger, these nerves release norepinephrine. Your heart beats faster and harder, blood vessels in your muscles dilate, and vessels in your digestive system constrict, redirecting blood where it’s needed most.
Parasympathetic nerves (primarily the vagus nerve) promote rest and recovery. They release acetylcholine, slowing your heart rate and reducing the force of contraction. This is why deep breathing and relaxation techniques can lower your heart rate—they stimulate vagal activity.
The cardiovascular control center in our brainstem integrates signals from baroreceptors, chemoreceptors (sensing oxygen and CO₂ levels), and higher brain regions. It constantly fine-tunes the balance between sympathetic and parasympathetic activity.
Hormonal Influences
Several hormones regulate cardiovascular function:
Epinephrine (adrenaline) from our adrenal glands reinforces sympathetic effects during stress, increasing heart rate and blood pressure dramatically.
Thyroid hormones increase our basal metabolic rate and cardiac output over weeks or months. Hyperthyroidism can cause a persistently rapid heartbeat.
Atrial natriuretic peptide (ANP) is released by stretched atrial cells when blood volume is too high. It promotes sodium and water loss through urine, reducing blood volume and pressure.
The renin-angiotensin-aldosterone system (RAAS) responds to low blood pressure or volume by conserving sodium and water while constricting vessels.
Response to Exercise and Stress
Exercise beautifully demonstrates cardiovascular coordination. Within seconds of starting to run:
Our heart rate increases from 70 to 150+ beats per minute. Stroke volume rises as our heart contracts more forcefully. Cardiac output can increase from 5 liters per minute at rest to 20+ liters during intense exercise.
Blood vessels in working muscles dilate dramatically, increasing flow 20-fold. Meanwhile, vessels in our digestive system and kidneys constrict, diverting blood to muscles.
Our breathing deepens and accelerates, increasing oxygen delivery to blood in our lungs. All these changes happen automatically, coordinated by our nervous and endocrine systems.
With regular exercise, our cardiovascular system becomes more efficient. Our resting heart rate drops, stroke volume increases, and our heart doesn’t have to work as hard for the same output.
Common Conditions Simplified
Understanding cardiovascular diseases helps us recognize symptoms early and appreciate why preventive care matters.
Hypertension: The Silent Pressure
High blood pressure affects nearly half of adults. It’s called the “silent killer” because most people feel fine despite dangerously elevated pressure damaging their arteries.
Normal blood pressure is below 120/80 mmHg. The first number (systolic) measures pressure during ventricular contraction. The second (diastolic) measures pressure during relaxation.
Chronic hypertension forces our heart to pump against increased resistance, thickening the left ventricle. It damages artery walls, accelerating atherosclerosis and increasing stroke and heart attack risk.
Most hypertension has no single cause. Genetics, excess salt intake, obesity, chronic stress, and aging all contribute. Treatment includes lifestyle changes (diet, exercise, stress management) and medications that reduce heart rate, dilate vessels, or decrease blood volume.
Coronary Artery Disease: When Supply Can’t Meet Demand
Your heart muscle needs constant oxygen delivery through coronary arteries. When these arteries narrow due to atherosclerosis (plaque buildup), oxygen supply becomes inadequate.
Initially, you might experience angina—chest pain or pressure during exertion when your heart demands more oxygen than narrowed arteries can deliver. Rest relieves the pain as demand drops.
If a plaque ruptures and triggers a blood clot, it can completely block a coronary artery, causing a heart attack (myocardial infarction). Heart muscle downstream from the blockage dies without oxygen. Quick treatment to restore flow is critical to minimize permanent damage.
Risk factors include smoking, high cholesterol, diabetes, hypertension, obesity, and family history. Prevention focuses on controlling these factors through medication, diet, exercise, and lifestyle changes.
Arrhythmias: When Rhythm Goes Wrong
Arrhythmias are abnormal heart rhythms caused by disrupted electrical signals. They range from harmless to life-threatening.
Atrial fibrillation is the most common serious arrhythmia. The atria quiver chaotically instead of contracting normally, reducing cardiac output and allowing blood to pool and clot. Stroke risk increases significantly because clots can travel to the brain.
Ventricular tachycardia is a rapid heart rate originating in the ventricles. It can deteriorate into ventricular fibrillation—chaotic, ineffective quivering that produces no cardiac output. Without immediate defibrillation, death occurs within minutes.
Bradycardia (slow heart rate) can result from SA node dysfunction or heart block (interrupted conduction). Severe cases require an artificial pacemaker.
Treatment depends on the type and severity. Options include medications, electrical cardioversion, catheter ablation (destroying problematic tissue), or implanted devices like pacemakers or defibrillators.
Heart Failure: When the Pump Weakens
Heart failure doesn’t mean our heart stops—it means it can’t pump efficiently enough to meet our body’s needs. This typically develops gradually after years of strain from hypertension, coronary disease, or valve problems.
Left-sided heart failure reduces blood flow throughout our body. Pressure backs up into our lungs, causing shortness of breath and fluid accumulation (pulmonary edema).
Right-sided heart failure allows blood to back up into our body, causing swelling in our legs, liver, and abdomen.
Symptoms include fatigue, shortness of breath (especially when lying flat), swelling, and reduced exercise tolerance. Treatment includes medications to reduce heart workload, manage fluid retention, and improve pumping efficiency. Severe cases may require mechanical assist devices or transplantation.
Conclusion
The cardiovascular system is a true masterpiece of biology. At a microscopic level, oxygen and carbon dioxide constantly exchange across tiny capillary walls. At the same time, perfectly timed electrical signals keep every heartbeat in sync. Each part plays its role, working together without pause.
When you understand heart blood flow and circulatory system anatomy, things start to click. You can spot warning signs earlier. You also see why everyday habits matter so much. For example, regular exercise trains your heart to pump stronger. A balanced diet helps keep blood vessels clear and flexible. Meanwhile, managing stress reduces the risk of long-term high blood pressure. And avoiding smoking protects your heart from serious, preventable damage.
In many ways, the cardiovascular system proves that the human body is more advanced than any machine ever created. Still, it isn’t invincible. It responds daily to the choices you make. Care for it consistently, and it will support you reliably for decades ahead.
Frequently Asked Questions
Our heart pumps approximately 2,000 gallons (7,500 liters) of blood through our body every day. That’s enough to fill a small swimming pool in just a few weeks.
The systolic pressure (top number) measures the force during ventricular contraction. The diastolic pressure (bottom number) measures residual pressure when the heart relaxes. Both numbers matter for assessing cardiovascular health.
A heart attack occurs when blocked coronary arteries prevent oxygen delivery to heart muscle. Cardiac arrest is when the heart suddenly stops beating effectively, usually due to electrical malfunction. Heart attacks can trigger cardiac arrest, but they’re distinct emergencies.
Regular exercise makes the heart more efficient, increasing stroke volume. An athletic heart pumps more blood per beat, so it needs fewer beats per minute to achieve the same cardiac output.
Recommended Resources for Curious Minds
As an Amazon Associate, we earn from qualifying purchases.
“The Heart: An Introduction to Cardiovascular Physiology” by Neil Herring This comprehensive textbook breaks down complex cardiac physiology into understandable concepts with excellent diagrams. Perfect for students or anyone wanting deeper scientific understanding beyond basic anatomy.
“Netter’s Cardiology” by Marschall S. Runge features the famous Netter anatomical illustrations showing the cardiovascular system in stunning detail. The visual approach makes complex structures and processes easier to grasp for visual learners.
3B Scientific Anatomical Heart Model A hands-on, life-sized model that separates into parts, showing chambers, valves, and vessels in three dimensions. Ideal for students or healthcare professionals who learn best by touching and manipulating physical structures.
“Heart: A History” by Sandeep Jauhar For those interested in the human side of cardiology, this book blends medical memoir with the fascinating history of how we learned about and learned to treat the heart. Accessible and engaging for general readers.
The information in this article is for educational purposes only and should not replace professional medical advice. Always consult with a healthcare provider for medical concerns.